|
Meadow Woods on Ebenezer’s Martin Luther Campus is an assisted living and memory care location that accepts Elderly Waiver. The Elderly Waiver Program in Minnesota provides for care services to seniors who do not have the assets and/or to pay for assisted living communities. At Ebenezer Martin Luther Campus, we are committed to the wellbeing of seniors navigating this process. Below is a starting place to find out if you may be eligible for this program and what it will cover for your care.
NOTE: The federal program called Medicaid is commonly referred to as Medical Assistance and Elderly Waiver in the state of Minnesota. Eligibility Requirements for the Elderly Waiver ProgramTo qualify for the Elderly Waiver program in Minnesota, there are three criteria that must be met by applicants:
Home Health Aide ServicesProvides for an on-going care plan with help for daily activities like bathing, dressing, grooming, light housekeeping, errands, and ambulating. In our assisted living environment, home health aides are available 24 hours, 7 days a week by call button. Meals and NutritionAll meals are provided at Meadow Woods Assisted Living with the Elderly Waiver. Activities A calendar of engaging activities, lifelong learning and spiritual care is available with Elderly Waiver. Specialized Medical Supplies and EquipmentFor seniors managing health conditions, Elderly Waiver often covers incontinence products, medical supplies, and assistive equipment like wheelchairs, walkers, and bath seats. Adult Day ServicesFor those who require supervision during the day, adult day programs at two locations, Martin Luther Campus and Creekside Community Center in Bloomington, provide socialization and assistance with medications while allowing regular caregivers a break. How to Apply for the Elderly Waiver ProgramSubmit Medical Assistance ApplicationCompleting the Medical Assistance application in the link below is the first step to apply. The application must be submitted to your county social services office. You will need to provide financial documentation to verify that you meet the income and asset guidelines. Instructions are provided in this Elderly Waiver MN program application. Complete AssessmentAfter submitting an application, a County nurse will come to your home to complete an in person assessment to evaluate health conditions, capabilities, and need for care services. The assessment determines if you require an assisted living level of care or other level. Get ApprovedFinally, the county will review your application and assessment to decide if you qualify for Elderly Waiver services. If approved, your county case worker will assist you in setting up care services to meet your needs. Costs and Coverage of Elderly Waiver ServicesIf you qualify and are enrolled, the Elderly Waiver program will cover service costs for your care that you cannot pay yourself at an Assisted Living. You will be required to pay for and manage any portion of rent and care as determined by the County at your income level. Selecting Elderly Waiver Providers and ServicesThe Elderly Waiver program allows participants to have a role in choosing service providers. Your county case worker can assist you in finding care providers where you may use Elderly Waiver and where it is accepted. You have the right to select your providers for services covered by your Elderly Waiver. Ongoing Eligibility Reviews and RequirementsAs an Elderly Waiver participant, your eligibility will be reviewed annually to ensure you still meet the requirements. Major life changes like increased income or changes in care level needed can impact ongoing eligibility. Additional Resources for the Elderly Waiver Program Navigating the Elderly Waiver Program can be complex, but resources exist to help answer your questions. The Senior Linkage Line has a website and phone number to answer questions. https://mn.gov/senior-linkage-line/ (800) 333-2433 Connecting with other elderly waiver participants can also provide useful insights to inform your experience. The Elderly Waiver provides a valuable benefit to seniors in need of care and support to continue living independently at home. Please reach out to us if you have any other questions! Contact Amy James, Sales and Outreach Director at Meadow Woods for more information at 952-885-8882 and amy.james@fairview.org
1 Comment
As we age, our bodies may become more susceptible to injury. According to the Centers for Disease Control and Prevention (CDC) in the United States, falls are the leading cause of injuries in older adults. Due to this, safety has become increasingly important in the education we provide for senior care in Bloomington. It is important to be aware of potential hazards and take steps to reduce the risk of injury to ensure we remain safe.
The senior population includes those aged 50 and up. This group comprises primarily pre-retirees and retirees who maintain an active lifestyle due to improved healthcare options, better nutrition, and technological advances. Some seniors may rely on support from family members or community resources to help them manage day-to-day tasks such as transportation and shopping for groceries. Those with disabilities may need an elderly disability waiver in Bloomington to ensure proper care. Care Options for Seniors Various services are available for older adults depending on their individual needs. For example, home care agencies or long-term care facilities like nursing homes or assisted living communities can help with daily activities such as bathing, dressing, and grooming. Additionally, recreational programs specifically designed for seniors promote physical activity, social interaction, and mental stimulation. These programs also offer an outlet for emotional support through peer counseling sessions or group therapy activities. The government also created elderly waiver programs in Bloomington for those who need funding assistance. There are hospice care programs for those nearing end-of-life and needing emotional comfort during their final days. Ways to Care for the Seniors at Home There are several ways to care for the seniors at home, including the following: Pay Attention When Walking When walking outdoors, you should wear comfortable shoes with good traction, such as low-heeled sneakers or rubber soles. Additionally, it's important to walk at a relaxed pace and pay attention to your footing. If possible, avoid walking on wet or icy surfaces, slippery floors, loose carpets or rugs, uneven pavement, or other potential tripping hazards. Keep Your Home Organized Clutter can create trip hazards in the home, so it's important to keep it organized and free from obstructions–especially on stairs and pathways between rooms. Make sure there is plenty of lighting throughout the home so you can easily see any obstacles that may be present. It might also help to use nightlights in hallways or bathrooms to prevent turning on brighter lights that may cause dizziness or disorientation when getting up at night. Exercise Regularly Regular exercise is a vital part of staying healthy for seniors, as it can help improve your balance, coordination, and strength, reducing risk of falling. Talk with a doctor about what types of exercise are appropriate based on the patient’s current health status. Patients who need help funding their treatments and exercise subscriptions may also qualify for the elderly waiver program in Bloomington. Use Assistive Devices Assistive devices such as grab bars in showers, canes, walkers in hallways, or handrails on staircases can provide additional stability when moving around your home or outside environment, thus reducing the risk of falls significantly. If needed, talk with your physician about whether these devices would benefit you based on your current level of mobility and stability. Install Security Systems Installing a security system is one of the essential safety tips for older adults. Security systems can monitor activity inside and outside the home and provide peace of mind knowing that help is available. Most security systems come with emergency alerts triggered by a push of a button when help is needed. Use Mobility Aids Mobility aids are essential for helping seniors maintain their independence while remaining safe at home or in public spaces. Mobility aids such as walkers, wheelchairs, scooters, and lifts can help reduce fall risks while providing an easier way to move indoors or outdoors. Identify Hazards Seniors and families may need to identify potential hazards in their homes or living environment that could cause injury or harm in some way. This includes items such as loose rugs and electrical cords that could be tripping hazards; furniture arrangement that could cause falls; poor lighting; slippery surfaces; sharp edges on furniture; etc. Once identified, it is important to reduce these hazards as much as possible by removing them from the environment or taking precautions when moving around them. Stay Connected Staying connected is critical to staying safe. Having friends who check in regularly or family members who are always available can go a long way towards reducing risks associated with being alone at home or out in public settings. Having someone available who can assist with grocery shopping, yard work, transportation needs, etc., can be very helpful in maintaining independence while always ensuring safety. Being aware of potential risks associated with aging can help older adults remain safe and independent while living on their terms. By implementing simple safety tips like using mobility aids, identifying potential hazardous areas within the home or living environment, and staying connected with friends and family, seniors can enjoy many years of living free from worry and fear. This year, Martin Luther Campus residents had the good fortune to be the recipient of a Service Project by our local Bloomington Girl Scouts - 9 Mile Service Unit! Over several months, more than 250 area girl scouts met and created May Day baskets and handwritten cards for the residents of Martin Luther Campus.
The baskets were crafted with paper cones and handmade arrangements of artificial flowers donated to Girl Scouts by area community members. The girls then wrote beautiful cards introducing themselves and sending warm wishes for Spring. In addition to being a wonderful gift for our older adults, these caring items created great conversations and joy. We hosted a social time for residents to receive the baskets and cards and to reminisce about their own involvement with Girl Scouts, Boy Scouts, Bluebirds, Campfire Girls and more. Some recalled being involved as a child or helping a sibling with their projects, while others were leaders for their own children’s troops. One resident dutifully recited her Girl Scout Troop number from childhood growing up in the Miami area (Troop 88). Then, her roommate remembered living in Missouri as an adult and helping many girls learn to camp as a Girl Scout leader. Residents remembered hiking and learning about the outdoors AND SELLING THE COOKIES. Everyone remembered the cookies with a smile! They even recalled when the price tag was around .50 cents a box! In addition to giving wonderful keepsakes that are now brightening resident rooms, this gift was intergenerational programming at it’s best…connecting seniors and young people together to learn from one another, to build a sense of community, and to enhance one another’s lives. Thank you, Bloomington Girl Scouts - 9Mile Service Unit, for the May Day Baskets. Your efforts meant so much to each and every resident...to know a little more about you and to know you care! Provided by Martin Luther Chaplain Linda At Martin Luther we continue to explore ways to support all members of our community on their journeys of life and faith. During April, three prominent religious traditions are observing significant holy days.
ISLAM – This year Muslims observe the holy month of Ramadan from April 2 - May 2.
Hydration is important! Liquids help us digest our food, get rid of waste, and absorb all the nutrients our body needs to thrive. As people get older, it can be more difficult to stay hydrated. Certain medications or health conditions can cause dehydration, and let’s be honest – it’s hard to drink the recommended six to eight glasses of water every day, even if you don’t have any compounding factors complicating things. If your loved one is having a hard time staying hydrated, it’s important to find a solution. Dehydration in seniors can cause or aggravate health problems and negatively impact quality of life. Luckily, staying hydrated doesn’t have to be difficult. Keep reading for a list of delicious and nutritious drinks that can help make hydrating a pleasure instead of a chore. Water If you’re aiming for hydration, nothing beats good, old-fashioned water. With that being said, water doesn’t have to be boring! Try shaking this classic up with a nutritious twist. Adding a slice of lemon or lime to a glass of water adds a splash of flavor. If your parents aren’t fans of citrus, cucumber or strawberry-infused water makes for a refreshing beverage. And if they like things on the sweet side, stir in a spoonful of honey for a healthier version of a sweetened drink. Smoothies Nothing says nutrition and hydration quite like a smoothie. While traditional fruit smoothies are undoubtedly delicious, try to talk mom and dad into giving a green smoothie a try. Green smoothies have veggies blended in, offering a host of additional nutrients for the same, fruity taste. Milk Milk is a superfood all on its own, containing almost every single nutrient that your body needs to thrive. Milk also happens to be a great source of vitamins that are especially helpful for seniors. Vitamin D and calcium help improve bone and muscle strength, and the mix of minerals in milk may even help improve blood pressure. If your mom or dad is lactose intolerant, there are numerous milk alternatives available that are also hydrating and nutritious. Green Tea If your parents are fans of tea, then make sure they give green tea a try. Not only does it help with hydration, but it’s also chock-full of antioxidants and natural compounds that help reduce inflammation, prevent cell damage, and even fight cancer. Juice While juice does come with a lot of sugar in the mix, fresh-pressed fruit and vegetable juices can be a great way to add hydration and nutrition to your parents’ day. Steer clear of juice concentrates when shopping at the store, and aim for products that advertise 100% juice with little or no added sugar. For an even healthier alternative, try making fresh juice yourself. There’s nothing more refreshing than a glass of fresh-pressed orange juice in the morning. If your loved one is having a hard time keeping up with their nutrition, a senior living community might be a good solution. At Martin Luther Senior Living & Care, we prioritize nutrition as part of our care. Learn more about our dining options by visiting the Dining and Culinary page on our website. Have you noticed a decrease in your Mom or Dad’s level of hygiene? Are they still wearing clothes they wore the day before – maybe even pants or a shirt that are visibly dirty? Is your parent’s hair often messier than usual? Is there discernible body odor where there wasn’t ever before?
As people age, some of the activities of daily living, like doing hair and makeup and even keeping up on laundry, can fall by the wayside. However, poor personal hygiene can also be a sign of a physical inability to complete everyday tasks, or it can be a sign of something more serious, such as dementia, memory loss, or another cognitive issue. For your loved one’s long-term health, it’s important to make a distinction between what they can improve on their own and what they may need more assistance with. Use these tips to talk to your loved one about what is going on, so you can ensure they get any extra assistance they may need and you can determine if a higher level of care is necessary. Start With the “Why” It’s quite possible your Mom or Dad doesn’t even know there is an issue. Maybe they let a particular hygiene activity go for a few days and before they realized, it was completely forgotten. Whether it was conscious or they are aware of the issue, it’s important to approach the question carefully, as many seniors are fearful of losing their independence. Using a calm, understanding voice, inform your loved one of the changes you have noticed. Don’t be accusatory or patronizing. Explain the Importance of Good Hygiene Frame the discussion around social expectations of what good hygiene is, again being careful to modulate your tone. If body odor is part of the issue, it can prevent people from wanting to visit your loved one, possibly leading to social isolation, which can cause a number of other compounding issues. Poor personal hygiene also has the potential to lead to skin irritation or infections, which can quickly snowball with older adults who are frail or have other underlying health problems. Ask How You Can Help! Does your loved one need an occasional reminder, more assistance with purchasing body care products, or do they just run out of time in the day? Moving slower can lead people to have trouble accomplishing everything they set out to do each day. Or your loved one could be depressed or anxious and in need of some counseling or medication. It can be good to include their doctor in this discussion, as well, to address any medically treatable concerns that may come up. Your loved one’s doctor also will know the right questions to ask in order to determine if your loved one is experiencing memory loss, dementia, or another cognitive issue. Together, you can determine if your loved one needs a higher level of assistance, such as home care, enhanced care, assisted living, or memory care. To learn more about all the care options available for your loved one at Martin Luther Campus in Bloomington, contact Amy James at 952-885-8882. Meadow Woods Assisted Living on the Martin Luther Campus is extremely proud to once again be voted THE BEST ASSISTED LIVING in Bloomington by local Sun Current readers. And Martin Luther Campus also received the BEST RETIREMENT COMMUNITY honor.
Each year, the Sun Current Newspapers asks members of our community to rate the local businesses and services that call Bloomington home, and we are delighted to be chosen! A heartfelt thank you for everyone who cast a vote for Martin Luther Campus. Our connections run deep with more than 60 years in this community, and we treasure all those who are a part of our Martin Luther Campus family. It is an honor and privilege for us to care for this community. Thank you. Meadow Woods also received the titles of Best Assisted Living and Best Memory Care in 2020 and 2021. As we get older, many of us want to stay in our homes as long as possible. But at some point, you may find that moving to a more supportive living environment is the right thing to do. Whether you're living alone and wishing for some companionship day to day, or need more help getting going in the morning and to bed at night, or finding that you'd rather not cook for yourself or do other household chores anymore, we've got a full gamut of options for you to explore.
At Martin Luther Campus, an Ebenezer senior living community, we've been a trusted leader in Bloomington, MN for more than 60 years. We offer assisted living, skilled nursing, memory care, and more. But, how do you know if it's time to make the move? If you’re starting to consider a move to a senior living community, here are some questions you may wish to ask yourself to determine if now is the right time. Am I lonely? This is a hard question to ask yourself, but loneliness is very common among seniors living in their own homes, especially if one spouse has passed away. Honestly, living alone day after day isn't all it's cracked up to be. But it doesn't have to be that way. Our senior living communities are teeming with opportunities for socialization and fun activities. You might be surprised at how much living in a community of people will enrich your life. Do daily activities seem like a burden? You may be just plain tired of cooking, doing the dishes or laundry and keeping the house as clean as you'd like it. Or you may find that tasks like dressing and bathing are a bit trickier now than they were when you were younger. Getting those buttons buttoned on your shirt can seem like an epic task, and you don't have to tell us how challenging it can be to put on your shoes some days. If you're nodding your head in agreement, it may be time to think about a senior community. We can help with all of that. When you move into senior living, much of that load is taken off your shoulders so you can relax and enjoy other elements of life. Do I spend days or weeks without leaving home? This question is less about loneliness and more about mobility, the physical act of leaving home and getting somewhere, like the grocery store or a friend's house. Have you stopped driving (usually because your kids have suggested it)? Are you having trouble getting up and down the stairs to the street or your garage? Is walking much more difficult now? If it's too difficult to get around, and you find it's just easier to stay home, this is one big indicator that a move to a senior community can greatly enrich your life. There's a lot going on in our senior living communities, and we can help you enjoy all of it. Have I had a health scare? Many times, moving to a senior community is precipitated by a health scare or, as your children may call it, a "teachable moment." If you've taken a fall at home, forgotten or been mixed up about your medications, been dizzy when sitting or standing, or if you have an ongoing health condition that will need to be monitored more than you can do yourself at home, you'll be more at ease in a community where everything is centered around your health and safety. Making the choice to move into senior living isn’t necessarily easy, but it’s OK to admit to yourself and others that you’ve reached a point where you need more support. Think about how such a move might give you greater calm, confidence and optimism as you begin the next stage of life. We at Martin Luther Campus are here to answer all your questions. Learn more by calling us at 952-888-8882. A few months ago, we welcomed Su-Yoon Ko to our campus virtually to host a community presentation on decluttering and bereavement organizing. Su-Yoon is a professional organizer and passionate about supporting clients in the physical and emotional process of looking at their things and determining what to keep.
Her calm, kind approach is both supportive and reassuring during what we all know can be a very difficult process. After her presentation, we asked Su-Yoon for a few good tips that someone trying to embark on a decluttering/organizing journey could hold close as they begin the process. Here are her words of wisdom... Decluttering. Where to Start? by: Su-Yoon Ko, Decluttering Key declutteringkey.com Decluttering is more than just about dealing with the physical stuff, it’s emotional, mental, and spiritual as well, not to mention if there’s the added layer of grief when you’re seeing to someone’s belongings who has died. There’s no rule that you have to keep anything at all, or that you have to let anything go- it’s about finding what works best for you. Here are a few tips. Journaling One way to start, before you even touch anything, is to journal. Spend some time thinking about the person you lost and free write, without judgement. What words or phrases would you use to describe them and your relationship with each other? What memories come up? Are there certain things that make you think of that person when you see them? Are these energetically uplifting for you? Relationships are complicated, and it’s not that we’re trying to deny anyone’s complexities, but it also doesn’t serve anyone to keep things that have a negative memory attached. If you start with an idea of what items help define that person to you, perhaps it’ll make it easier to let go of the items that don’t have that same energy of memory for you. Set the boundaries Taking your unique situation into consideration, what do you truly have space for? If you have a boundary set in place before you get into the actual physical items, it might be easier to make decisions. What feels right to you: keep whatever fits in this closet? On this shelf? Or in this box? There’s no right or wrong, just what’s right or wrong for you. Setting boundaries will help give you clarity as you move through items. Will there be exceptions? Certainly; being flexible enough to consider those on a case by case basis can bring some peace. Pre-Sort Here’s a familiar scenario: you start sorting books, then you see a shoe and think “I’ll just put it in the closet”, you open the closet and start arranging clothes and suddenly you think “Wait what was I doing?” It’s easy to get distracted and never quite finish the task you started. One thing to do, you or someone who wants to help, is to pre-sort. This means putting all similar items together (“like with like” as professional organizers say), for example all paperwork together, books with books, etc. I feel that putting like with like from the whole house in one place works best; if that’s not be possible, then pre-sort room by room. After pre-sorting, it’s easier for the decision maker to then sort into keep, donate, sell etc. piles without distracting items. Intentionally saved vs. not decluttered When seeing to someone else’s belongings after they die, it can be difficult to let anything go, especially in the midst of grief. Reframing your perspective that many of the items there were perhaps not intentionally saved, rather they just had not yet been dealt with - sorted and taken to donation, trash or in general decluttered in some way, could be helpful. Trust that you’ll be able to discern what is truly a treasure and worth your time and effort to deal thoughtfully with, and what is not. Q & A with the Deceased Not that you need permission to let go of things that don’t fit your life, a suggestion if you do seek that extra support, is directly asking the deceased. Connect with them energetically and ask - aloud or in your mind – (“Grandma, is it ok if I let this afghan go?”, “Dad, would it be ok if I gave this book away?”), and then just listen for any thoughts or feelings that come to you. Quite often people hear in their mind an answer. This has been immensely helpful for some clients, and not so much for others. It’s just another tool in your toolbelt that you can pull out and use if the situation feels right. Need help getting started with your decluttering project? Contact Su-Yoon directly to learn more about her services at: declutteringkey.com/contact Martin Luther Care Center is part of the Ebenezer family of Senior Care Communities. We provide transitional care, long term care, assisted living apartments, and memory care for seniors in Bloomington, Minnesota. We also have adult day programs for seniors living at home. We’re located at 1401 East 100th St., in Bloomington, MN. Are you or a loved one interested in learning more about assisted living care? Call Amy at 952-885-8882 or more information and to schedule a tour today. By Sally Peterson, Director of Community Programs Happy National Volunteer Appreciation Week to you, our valued volunteers!
We want to recognize that our volunteers continue to be a vital part of the Martin Luther Campus fabric. While we continue to be living through unprecedented times, it does not mean that your continued commitment to Martin Luther Campus as a volunteer has gone unnoticed. During the past year, many of our volunteers have found ways to volunteer from afar. At a time when our residents were more isolated, these efforts have been critical and so appreciated. Homemade masks, cards, letters, treats, bingo prizes, lap robes, phone calls, cutting/prepping for projects, donations, books, and check-ins…the list goes on and on. What a difference you have made! We miss seeing you so much, but know you continue to be with us in spirit. We appreciate you as much as always and look forward to welcoming you back on campus doing what you do best . . .caring for others! |
Director of Community Relations
Hello friends, my name is Kate and I'd love to share with you ALL of the wonderful things happening at Martin Luther Campus. Be sure to check our Blog, Lifestyle page and Facebook page often to stay updated on the happenings at our community! Archives
November 2023
Categories |
|
telephone |
|
DIRECTIONSimap
|
© 2021 Fairview Health Services
|






















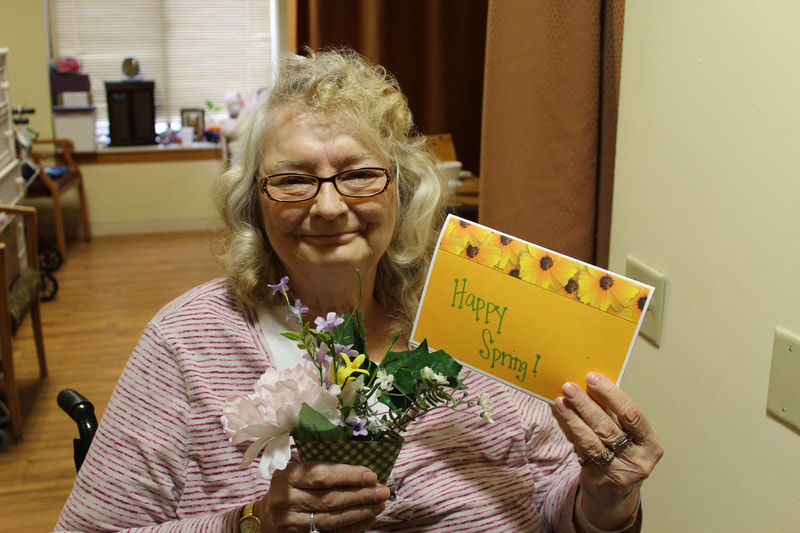








 RSS Feed
RSS Feed

